Understanding CPAP in the NICU: A Parent’s Guide to Breathing Support
As a NICU parent, seeing your baby connected to equipment can feel overwhelming. One of the most common forms of breathing support you may see is CPAP. If your baby is on CPAP, you are not alone - and understanding it can help ease of some of the fear.
Let’s walk through what CPAP is, why it is used, and what it means for your baby.
CPAP stands for Continuous Positive Airway Pressure.
It is a gentle form of breathing support that delivers a steady flow of air (sometimes with oxygen) into your baby’s nose to help keep their lungs open.
Unlike a ventilator, CPAP:
Does not breathe for your baby
Does not require a breathing tube down the throat
Allows your baby to breathe on their own
Think of it like a small air “splint” that keeps tiny air sacs (alveoli) from collapsing between breaths.
Why do NICU babies need CPAP?
Many premature babies need extra breathing support because their lungs are still developing.
CPAP is commonly used for:
Prematurity
Mild to moderate Respirtory Distress Syndrome (RDS)
After being removed from a ventilator
Apnea of prematurity (pauses in breathing)
To help keep oxygen levels stable
Preterm lungs can collapse easily. CPAP helps prevent that collapse making breathing less tiring.
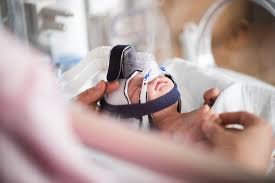
What does CPAP look like?
You may see:
Small nasal prongs sitting in your baby’s nostrils
Or a small mask that rests over the nose
A soft hat that helps keep the tubing in place
Tubing connected to a CPAP machine or ventilator
Monitors that track oxygen, Heart rate and breathing
A small tube that goes from the mouth to the stomach that will help evacuate air from the stomach. This can also be used for feeding until they come off CPAP.
It can look like a lot - but each piece has a purpose.
Is CPAP painful?
CPAP itself is not painful.
However, because the prongs sit in the nose, babies can sometimes develop:
mild nasal irritation
skin redness
pressure areas
Your NICU team carefully checks your babies skin and adjusts the equipment to prevent injury.
Can I hold my Baby on CPAP?
In many NICU’s - yes.
Babies on CPAP can often:
Do skin-to-skin (kangaroo care)
Be gently held
Participate in care times
Always ask your nurse. Holding your baby is still incredibly important for bonding and development.
How long will my baby need CPAP?
Every baby is different.
Some babies need CPAP for:
a few days
a few weeks
sometimes longer depending on their gestational age and lung maturity
As you baby grows stronger, the team will slowly decrease the pressure or oxygen. This is called weaning.
Progress in the NICU is rarely perfectly linear. Small setbacks are normal.
What Parents Often Worry About
“Will this hurt their lungs?”
No - CPAP is designed to protect and support fragile lungs.
“Does this mean my baby is very sick?”
Not necessarily. Many preemies need CPAP simply because they were born early. It is a very common intervention for even term babies in the NICU.
“Will they have long-term breathing problems?”
Most babies outgrow the need for CPAP as their lungs mature or heal.
Questions You Can Ask Your NICU Team
What CPAP setting is my baby on?
How much oxygen are they receiving?
What signs show they are ready to wean?
Can I participate in care while my baby is on CPAP?
Knowledge builds confidence. And confident parents feel less helpless.
A Gentle Reminder for Parents
If your baby is on CPAP righ now, here is what matters:
Your baby is breathing
Your baby is growing
Your baby is fighting - and CPAP is helping
The machines can fee scary but they are tools - not barriers between you and your baby.