Your Baby is in the NICU: What Happens Next?
By Jeri, Neonatal Nurse Practitioner | Bright Sprout
Bringing a baby into the world is supposed to feel joyful and simple.
When your baby is admitted to the Neonatal Intensive Care Unit (NICU), everything changes.
If you’re reading this, you may feel overwhelmed, scared, numb - or all three. I’ve worked in the NICU for more than 25 years, first as a nurse and now as a Neonatal Nurse Practitioner. Let me gently walk you through what happens next.
What is the NICU?
The NICU is a specialized unit designed to care for babies who need extra support after birth.
Babies may be admitted because they were:
Born premature
Having breathing difficulties
Small for gestational age
Fighting infections
Needing monitoring after delivery complications
Some stays are brief. Some are longer. Every baby’s journey is different.
Who is taking care of your baby?
Your baby’s team may include:
Neonatal Nurse Practitioners (like me)
Neonatologists (NICU doctors)
Bedside NICU nurses
Respiratory Therapists
Lactation Consultants
Physical, occupational, and speech therapists
Social workers
YOU are also part of this team!
You are NOT in the way.
You are NOT bothering us.
You DO belong at your baby’s bedside.
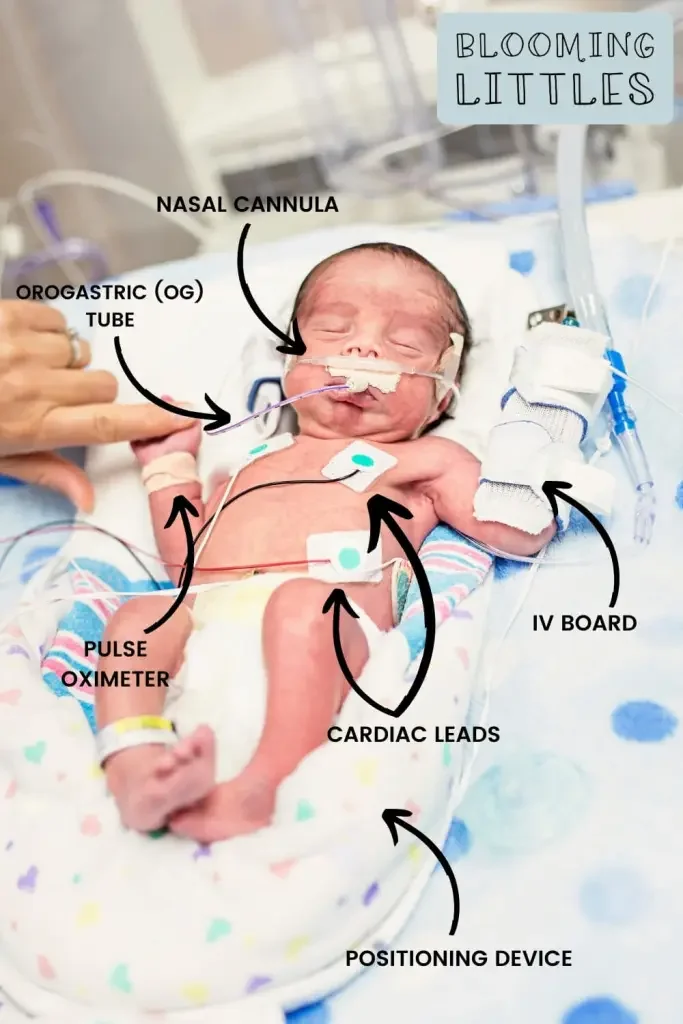
Why Does My Baby Have So Many Wires?
NICU equipment can look intimidating at first. Here is what you may see:
CPAP (Breathing support)
CPAP helps keep your baby’s lungs gently open while they breathe on their own. It is not painful. It provides steady air pressure to prevent tiny air sacs (called aveoli) from collapsing.
Many preterm babies need this temporarily and also as support when weaning off the ventilator.
Feeding Tube
Premature babies often don’t yet have the coordination to suck, swallow, and breathe safely. A small tube delivers milk directly to the stomach until they are ready. This tube will also help prevent air from building up in the stomach causing discomfort. All babies that are placed on CPAP, including term newborns, will need to have this tube to help evacuate air from the stomach and also to start feedings that would be unsafe to be given via bottle or breast while they are on this support.
This is developmental and for safety and is not a setback.
Monitoring Leads
The monitors trach heart rate, breathing, and oxygen levels. Alarms sound frequently - many are reminders, not emergencies.
Your team knows the difference.
What Can You Do Right Now?
You may feel helpless. You are not.
Here are powerful things only you can do:
Place your hand gently on your baby. Still touch is calming. Ask your nurse what is appropriate for your baby
Provide breast milk if possible
Read or talk slowly and softly to your baby - they know your voice
Participate in care times
Practice Kangaroo care when medically appropriate
Touch matters. Your voice matters. YOU matter.
How Long Will My Baby Stay?
One of the hardest answers in the NICU is “It Depends.”
As a general guideline, many premature babies go home around their original due date - but that varies.
Instead of focusing on the finish line, we focus on:
Breathing independently
Feeding consistently
Maintaining temperature
Growing steadily
Progress in the NICU is rarely linear. Two steps forward, one step back is common.
A Word from My Heart
I have cared for thousands of NICU families.
The parents who struggle the most are often the ones who feel they must “be strong”.
You are allowed to feel everything.
The NICU is not the beginning you planned. But it can still become a story of strength, resilience, and deep connection.
Gentle Support for the Journey
Many parents tell me they forget details because survival mode takes over.
That is one reason I created the Bright Sprout NICU journal - a place to record milestones, emotions, and small victories that might otherwise blur together.
Because even in the NICU…tiny beginnings bloom.
Feeling overwhelmed?
Download my free “First 7 Days in the NICU” Survival Checklist to help you feel more confident and organized during your stay.